Free express quote
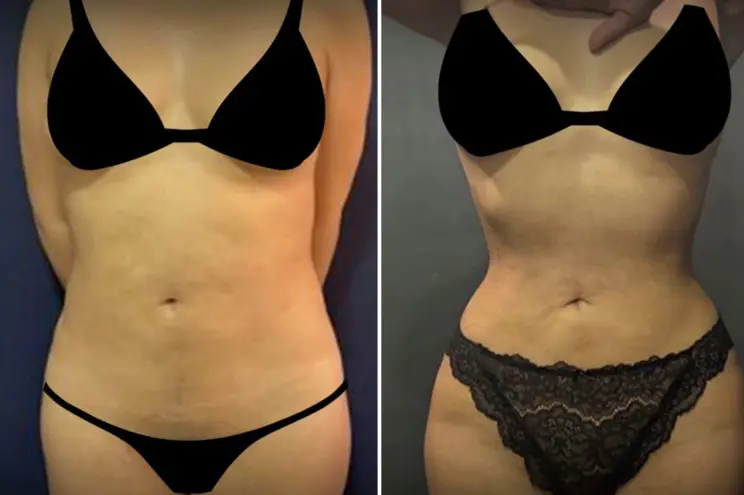
The RIBXCAR post-operative protocol can feel, in the first few days, like a heavy set of constraints to bear. Three months in a brace, a week of relative immobility, dozens of daily spirometry cycles, dietary restrictions, precise medication schedules — all of this demands genuine effort and sustained discipline.
What is RIBXCAR?
The term RIBXCAR refers to a three-dimensional thoracic remodeling surgical protocol developed by Dr. Youssef Gam. Its name synthesizes two fundamental anatomical and clinical realities: rib, a direct reference to the cartilaginous structures being worked on, and scar, a reminder that any intervention of this nature must result in minimized and controlled scarring.
This is neither a classic liposuction nor an abdominoplasty: the RIBXCAR procedure acts deep within the rib cage itself, remodeling the costal cartilages to slim the waist, redefine the costal arches, and harmonize the overall volume of the trunk. Candidates for this procedure vary widely: some seek a pronounced feminine curve, others a morphological correction related to asymmetry or an unsatisfactory thoracic shape.
What sets RIBXCAR apart from other thoracic sculpting approaches lies in the combination of three elements: rigorous preoperative digital planning, millimeter-precise surgical technique, and a structured post-operative protocol whose adherence directly determines the quality and durability of the result.
Surgical Planning: 3D Mapping
Before any incision, Dr. Gam carries out a three-dimensional mapping of the patient’s rib cage. This modeling, produced from medical imaging data, relies on a tool referred to in the protocol as the 3D Rib Grill Tem with Cartilagennel Vent.
This personalized volumetric representation allows several key parameters to be identified before the operation:
- The exact position and thickness of the lower costal arches;
- Natural left/right asymmetries of the rib cage;
- Predictable tension zones following resection or remodeling;
- The aesthetic projection of the result from different angles.
This planning is not a formality. It determines the number and location of surgical gestures, the volume of tissue removed or modified, and the orientation of incisions. The patient is involved in this decision-making phase, which deepens their understanding of the surgical procedure and facilitates their commitment to post-operative follow-up.
“A well-planned surgery is already half done. The rest is decided in the weeks that follow.”
— Dr. Youssef Gam
Week 1: Strict Rest and Controlled Mobilization
The first seven post-operative days represent the most critical phase of recovery. During this window, the remodeled costal cartilages are at their most vulnerable: consolidation has not yet begun and they are extremely sensitive to external mechanical forces.
Strictly Forbidden During the First 7 Days:
- Getting up or lying down abruptly;
- Climbing or descending stairs;
- Carrying objects, even light ones;
- Bending forward or rotating the trunk.
Forbidden During the First 2 Weeks:
- Any physical exertion, regardless of intensity level;
- Any form of sport or athletic activity.
These restrictions are grounded in the physiology of cartilage healing. Unlike skin or muscle, cartilage is poorly vascularized. Its repair cells — chondrocytes — work slowly and cannot tolerate any excessive mechanical stress in the early phase. A sudden movement is enough to cause a microtrauma that will delay consolidation by several weeks.
When walking is gradually permitted, it must be done slowly, with assistance, and with the gaze directed straight ahead. This posture prevents lateral tilting that exerts traction on the thoracic walls.
The Thoracic Brace: Three Months of Progressive Compression
Wearing a thoracic compression brace is one of the cornerstones of the RIBXCAR protocol. It is worn 24 hours a day, 7 days a week, for 3 consecutive months. Neither sleep nor bathing constitutes a valid exception to this rule.
Why So Long?
The three-month duration corresponds precisely to the time needed for the remodeled cartilages to complete their primary consolidation phase. During this period, the brace simultaneously fulfills several functions:
- Positional support
- It holds the cartilages in the position intended by the surgeon, preventing any displacement caused by respiratory movements.
- Seroma reduction
- Mechanical compression limits the accumulation of fluid in the spaces created by the surgical procedure.
- Skin retraction
- It encourages the progressive adaptation of the skin to the new thoracic morphology.
- Scar stabilization
- It reduces tension on the suture lines and lowers the risk of hypertrophic scarring.
Progressive Reduction: 1 cm Per Week
The brace is not removed all at once at the end of three months. It is loosened by one centimeter per week, allowing the tissues to gradually adapt to the reduction in external pressure. This progressive loosening replicates the natural retraction of tissues and prevents morphological “rebound.”
Important: it is forbidden to remove or modify the brace on your own initiative. In the event of pain, skin irritation, or discomfort, the only appropriate course of action is to contact Dr. Gam’s office directly for a supervised adjustment.
Diet, Hydration, and Restrictions
Post-operative recovery is not played out solely in the recovery room or under the compression brace. It also unfolds on the plate. The RIBXCAR protocol assigns a central role to nutrition, viewing it as an active lever in the healing process.
Positive Recommendations
| Category | Detail | Justification |
|---|---|---|
| Proteins | Poultry, eggs, legumes, dairy products | Collagen synthesis and tissue repair |
| Hydration | Minimum 3 liters of water per day | Elimination of metabolic waste, thromboembolic prevention |
| Vitamins | Fresh fruits and vegetables | Vitamin C intake, a cofactor in collagen synthesis |
Strict Dietary Prohibitions
- Chili peppers and strong spices — promote inflammatory responses and exacerbate pain;
- Shellfish — high allergenic potential and histamine content incompatible with active healing;
- Pork — pro-inflammatory under certain post-surgical metabolic conditions;
- Fish (certain species) — variable histamine content depending on freshness and species.
Substances Prohibited for 1 Month
- Tobacco: nicotine causes vasoconstriction, depriving healing tissues of oxygen and nutrients;
- Alcohol: disrupts coagulation, increases hemorrhagic risk, and amplifies the sedative effects of post-operative medications.
Breathing Exercises and Vascular Prevention
Two series of exercises are prescribed in the RIBXCAR protocol to prevent potentially serious complications related to post-operative immobility.
Incentive Spirometry
An incentive spirometer is a small medical device that the patient inhales through to raise a ball or piston as high as possible. The protocol prescribes 20 repetitions every 4 hours.
After thoracic surgery, pain naturally encourages shallow breathing to avoid engaging the operated areas. This avoidance strategy, while understandable, leads to under-ventilation of the lung bases, which can result in atelectasis — areas of lung tissue that collapse from lack of ventilation — and, in the most unfavorable cases, infectious pneumonia. Spirometry breaks this vicious cycle by forcing a deep, active inspiration.
Limb Mobilization
While lying down, the patient is asked to regularly and continuously mobilize their hands, arms, legs, and feet.
These movements, even of small amplitude, maintain venous blood flow in the lower limbs. Prolonged immobilization slows this flow and promotes the formation of deep venous thrombi which, if dislodged, can cause pulmonary embolism. This complication, while rare, is one of the most serious in surgical post-operative care. Regular mobilization is the best prophylaxis.
Sleeping Correctly After Surgery
Sleep position is a variable often overlooked by patients but considered decisive in the RIBXCAR protocol.
It is mandatory to sleep on your back (dorsal position) throughout the entire active healing phase. Side (lateral) and stomach (prone) positions are strictly prohibited.
Why This Requirement?
- Sleeping on your side exerts unilateral compression on the cartilages that have just been remodeled, risking asymmetric deformation of the result;
- Sleeping on your stomach compresses the entire anterior surface of the thorax, compromising the stability of the operated areas;
- The dorsal position guarantees symmetrical ventilation of both lungs and reduces all tension on the scars.
For patients accustomed to sleeping on their side or stomach, using positional pillows on either side of the body can help maintain the dorsal position throughout the night.
Normal Signs Versus Emergency Signs
An important part of the RIBXCAR protocol involves educating patients about what is normal to observe after the procedure, and what should, on the contrary, prompt immediate concern.
Normal Manifestations, Not Requiring Emergency Consultation:
- Swelling of the extremities (edema): a natural inflammatory response to the surgical act and the temporary reduction in physical activity. It resolves spontaneously with the progressive resumption of mobility and good hydration.
- Sensations of cracking or thoracic movement: these clicks correspond to the normal micro-movements of cartilages in the consolidation phase. They do not indicate displacement or rupture. They are analogous to the ordinary joint sounds anyone can produce when stretching.
Warning Signs Requiring Immediate Consultation:
| Sign | Possible Cause | Course of Action |
|---|---|---|
| Fever > 39°C (102.2°F) | Post-operative infection, pneumonia, systemic complication | Immediate call to the office, emergency room if necessary |
| Loss of consciousness | Pulmonary embolism, severe hypotension, cardiovascular disorder | Immediate call to emergency services |
Prescribed Medications: Role and Schedule
The post-operative medication protocol runs for 7 days and is based on four complementary molecules, prescribed at precise times to optimize their action and limit interactions.
| Medication | Dosage | Schedule | Primary Role |
|---|---|---|---|
| Lansoprazole 30 mg | 1 tablet | 6:00 AM, on an empty stomach | Gastric protection (proton pump inhibitor) |
| Arcoxia 60 mg (etoricoxib) | 1 tablet | Every 12 hours, with food | Anti-inflammatory and analgesic (selective COX-2 NSAID) |
| Paracetamol 500 mg | 1 tablet | Every 8 hours | Complementary central analgesic |
| Cefuroxime 500 mg | 1 tablet | Every 12 hours | Preventive antibiotic (2nd-generation cephalosporin) |
Important Notes on the Prescription
- Lansoprazole protects the stomach lining from the irritating effects of Arcoxia; it must be taken before the other medications, on an empty stomach.
- The Arcoxia + Paracetamol combination constitutes multimodal analgesia: the two molecules act via different mechanisms and mutually potentiate each other.
- Cefuroxime must not be interrupted before the end of 7 days, even in the absence of apparent signs of infection.
- In case of doubt about an allergy or drug interaction, contact the office without delay.
The Post-Operative Follow-Up Consultation
A check-up consultation is integrated into the RIBXCAR care pathway. It is a strategic moment allowing Dr. Gam to evaluate the progression of healing, adjust the compression brace if necessary, and answer the patient’s questions.
What the Patient Must Bring to This Consultation:
- A fitted shirt or bodysuit to allow a precise morphological assessment under real conditions;
- A healing cream such as Biafine or Bépanthène, which will be applied to the scars during the consultation.
Why Biafine or Bépanthène?
These two emollients have complementary properties in scar maturation:
- Biafine: particularly effective on recent scars and areas of tension; reduces local inflammatory reaction and deeply moisturizes;
- Bépanthène (provitamin B5): promotes epithelial regeneration, maintains skin hydration, and improves the suppleness of the forming scar.
Their regular application at home, following Dr. Gam’s instructions, helps reduce the risk of hypertrophic or keloid scarring.
Why Following This Protocol Changes Everything
The RIBXCAR post-operative protocol can feel, in the first few days, like a heavy set of constraints to bear. Three months in a brace, a week of relative immobility, dozens of daily spirometry cycles, dietary restrictions, precise medication schedules — all of this demands genuine effort and sustained discipline.
Yet every element of this protocol responds to a precise medical rationale, built from Dr. Gam’s clinical experience and the data of cartilage healing physiology. There is no arbitrary recommendation in this document.
What is at stake in these three post-operative months is the permanence of the result. A remodeled cartilage that heals under poor mechanical conditions may return to an undesired position, produce excessive fibrosis, or generate secondary asymmetries. Conversely, a cartilage that consolidates in a stable environment — well compressed, properly nourished, and protected from infection — becomes a definitive structure that will preserve the aesthetic result for years to come.
In this sense, the RIBXCAR patient is not a passive subject submitting to a surgeon’s decisions: they are an indispensable co-actor in their own outcome. The operating room is only the beginning. The real work starts the next morning — brace firmly fastened, spirometer in hand, glass of water on the bedside table.
Any question relating to your post-operative health should be addressed directly to Dr. Youssef Gam or his team.
